The Benefits and Challenges of Mental Health Consultation
Consultation within the context of mental health is something every therapist should be familiar with and engage in--yet there is this anxious...
3 min read
 Monet David, MS, LPC
:
Dec 5, 2023 11:39:35 AM
Monet David, MS, LPC
:
Dec 5, 2023 11:39:35 AM

As I continue to evolve in my professional identity, a lingering question has begun to consume my thoughts. Despite the extensive training and education that Counselor Education graduate students receive, along with the emphasis on ethical considerations and best practices, there remains a stark contrast between theory and practice. This dichotomy has led me to ponder: what if I have unintentionally caused harm to my clients?
When deferring to the American Counseling Association's Code of Ethics we are immediately met with this lovely preamble,
"These principles are the foundation for ethical behavior and decision making. The fundamental principles of professional ethical behavior are
• autonomy, or fostering the right to control the direction of one’s life;
• nonmaleficence, or avoiding actions that cause harm;
• beneficence, or working for the good of the individual and society by promoting mental health and well-being;
• justice, or treating individuals equitably and fostering fairness and equality;
• fidelity, or honoring commitments and keeping promises, including fulfilling one’s responsibilities of trust in professional relationships; and
• veracity, or dealing truthfully with individuals with whom counselors come into professional contact."
Further into the document it goes into greater detail of potential harmful behavior that can be enacted by therapists (e.g., imposing your own personal values onto a client, engaging in a dual relationship with a client, or even providing therapeutic services to a friend or family member). The code also discusses other gray areas including bartering for services and receiving gifts from clients. Of course, they emphasize taking every precaution to avoid breaches of confidentiality. But what about good intentions gone awry? What if in our best efforts to abide by nonmaleficence we end up causing harm anyway?
Prior to working in private practice I served as an Assessment Therapist for a community agency that worked solely with Medicaid recipients. My job was to assess each potential client for evidenced based services and justify said services were worthy of being compensated by Medicaid. Medicaid in Louisiana is, if anything, infamous for their temperamental approval of any mental health services.
This is where my curiosity around harm has been brewing. The overall attitude towards diagnosis in graduate school is that you must meet with your client for several sessions before you can truly have an adequate diagnostic impression. In the real world, most insurance companies (both Medicaid and private alike) want a diagnosis within the first appointment. Okay, then we are taught to provide the "least harmful" diagnosis to offset any additional stigma or shame the client may be experiencing. Once again, good idea in theory. Poor in application.
This was my own experience--so perhaps other therapists have experienced something very different. More often than not the clients I assessed were mandated (read; forced to attend therapy) either through the juvenile justice or foster care system. Diagnostically, it was incredibly difficult to create a snapshot of how they came to be referred for therapeutic services. It quickly became evident that behaviors being enacted by these kiddos were more attributable to circumstance rather than pathology. In an effort to not cause additional harm I would feel compelled to diagnose with the ever-popular, "Adjustment Disorder" (this diagnosis serves as a lovely catch-all to describe one's experience dealing with repercussions of an event that has taken place in their life within the last 6 months). However, I was met with feedback that this diagnosis was not strong enough to warrant the type of therapy the client would be participating in. I needed to rely on "heavier" diagnoses to really make a case for evidenced based intervention.
But is it appropriate and least harmful to give a kid a diagnosis of Oppositional Defiant Disorder when in reality their behaviors are better contextualized through a trauma lens or even Neurodivergence? To this day, I still don't have a confident answer. I know I eventually left that job because it was hard to reconcile that families were being forced to attend therapy when their basic needs weren't being met. How could I ask a family to process their complex trauma when they were still living it on a daily basis? It felt beyond harmful--cruel even.
But maybe I'm being hyperbolic. Maybe the work I was contributing to was helpful. My professors worked so hard to help me understand the deeply nuanced nature of therapy from day one of graduate school. I don't think you can prepare anyone for this type of ambiguity. It can't be taught. Just experienced. Vicarious trauma. A lot of introspection about the work you do and if it's even worth it some days.
That looks like consistent consultation, reflection and continuing education. I can't ever know enough because the human experience is dynamic and ever shifting. The minute I feel I know everything I've lost. It's also remaining humble and curious. Being accountable to myself, my profession and my clients. Therapists have goofed a lot of things in the past and probably even now but from those mistakes come lessons and the ability to correct.
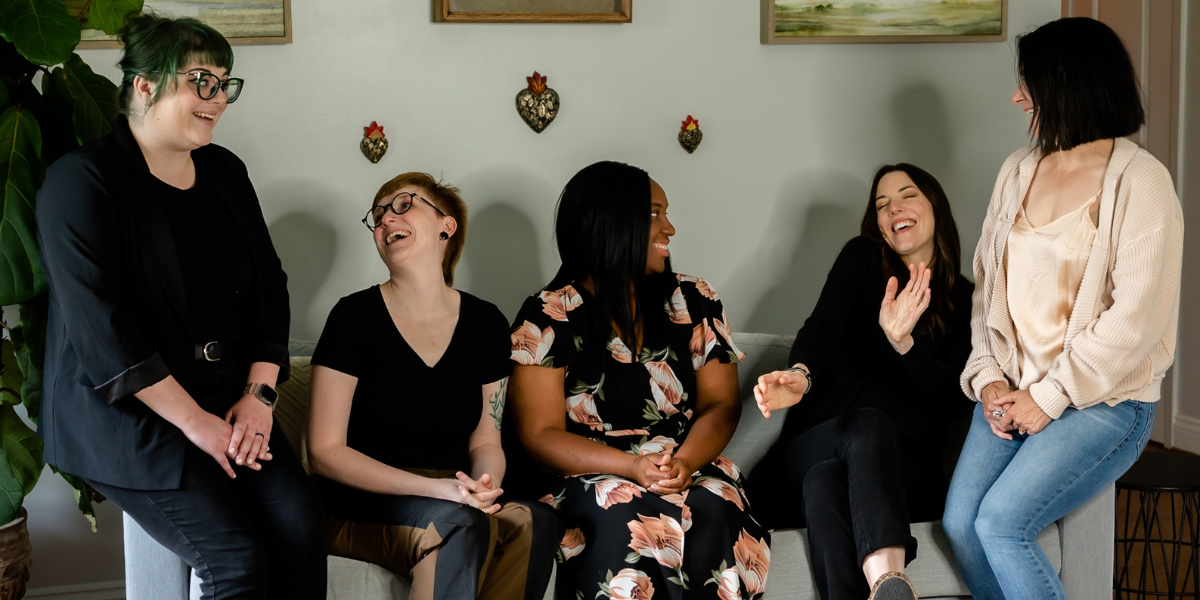
Consultation within the context of mental health is something every therapist should be familiar with and engage in--yet there is this anxious...

In working with a diverse range of helping professionals, including undergraduate psychology students, fellow counselors (and other mental health...
-1.png)
As mental health therapists, we are trained to understand and address distress and to help our clients navigate their inner worlds and external...