Differentiating OCD and Anxiety Disorders
For therapists, grasping the nuanced distinctions between OCD and other anxiety disorders is vital for accurate diagnosis, leading to the most...
2 min read
KD Holmes, LPC
:
Jun 29, 2023 4:06:49 PM

As a therapist, one of the most important things we can do for our clients is to provide trauma-informed care, and it is specifically useful with neurodivergent individuals. Many people struggle with the impact of trauma and are neurodivergent. Trauma symptoms and neurodivergent differences overlap making it difficult to differentiate between the two. This overlap makes the path to healing different so we must be neurodivergent informed to provide effective solutions. Let's take a closer look at the complex relationship between trauma and neurodivergence, and how we, therapists, can help our clients navigate this intersection.
Individuals who are Autistic are more susceptible to exposure to adversity and violence, raising the likelihood of experiencing trauma. The statistics on this are alarming. While autism and trauma share symptoms such as isolation and intense sensory experiences, it is crucial to distinguish between the two. When working with Autistic clients, an understanding of their neuro cognitive perspective is necessary. Using individualized treatment for each client with autism and trauma leads to a greater acceptance of self, and better outcomes due to more authentic living.
There are lots of clients that have traits of Autism without having the diagnosis and these traits also must be considered when treating trauma. Specific importance must be given to sensory differences. Understanding these differences is at the core of what we do in the therapy room, because sensory differences dictate which coping strategies will be effective.
Attention-deficit/hyperactivity disorder (ADHD) frequently co-occurs with trauma. As a therapist, identifying the accurate diagnosis can be a significant challenge, as the symptoms of both conditions overlap. While ongoing research attempts to understand the overlap between ADHD and trauma, a customized and targeted approach to treatment that addresses individual trauma experiences and ADHD symptoms will provide the best outcomes for our clients. This population is also more likely to experience poly victimization as well. So if someone has ADHD we must also explore their trauma history.
Individuals with autism are three times more likely to experience dissociative symptoms than their neurotypical peers. This co-occurrences of symptoms has to be considered when treating trauma. Helping autistic clients identify dissociation and its correlation, is essential to their wellbeing. Stabilization Techniques are helpful to clients experiencing dissociative states but these techniques rest on the foundation of sensory differences. These differences must be identified to find effective neurodivergent stabilization skills.
Alexithymia is common among individuals with dissociative experiences. Alexithymia refers to a difficulty in verbalizing one's emotions to oneself or others. Alexithymia and dissociation both involve disruptions in awareness and emotional regulation. People with alexithymia have difficulty recognizing and articulating their emotional experiences, and dissociation is the disconnection or separation from conscious awareness from memories or emotions. We as therapists need to differentiate between alexithymia and dissociative experiences. We need more education on this to effectively treat both. Alexithymia has poor outcomes in therapy and effective treatment consists of skills focused on identifying and verbally expressing emotions, and understanding the mind–body connection. This will look different for people with Alexithymia so our Neurotypical expectations need to be kept in check.
Assisting clients with a trauma history and neurodivergence differences requires a heightened awareness of the specific intersection between both sets of symptoms. Clients need individualized treatment interventions that focus on assessing their unique situations and sensory differences. Offering integrated treatment for the overlap can lead to more acceptance of self and more effective coping. Acknowledging and addressing the overlap between trauma and neurodivergence is crucial to assist clients in identifying solutions that work.
Check out our CE on Trauma Informed Therapy!
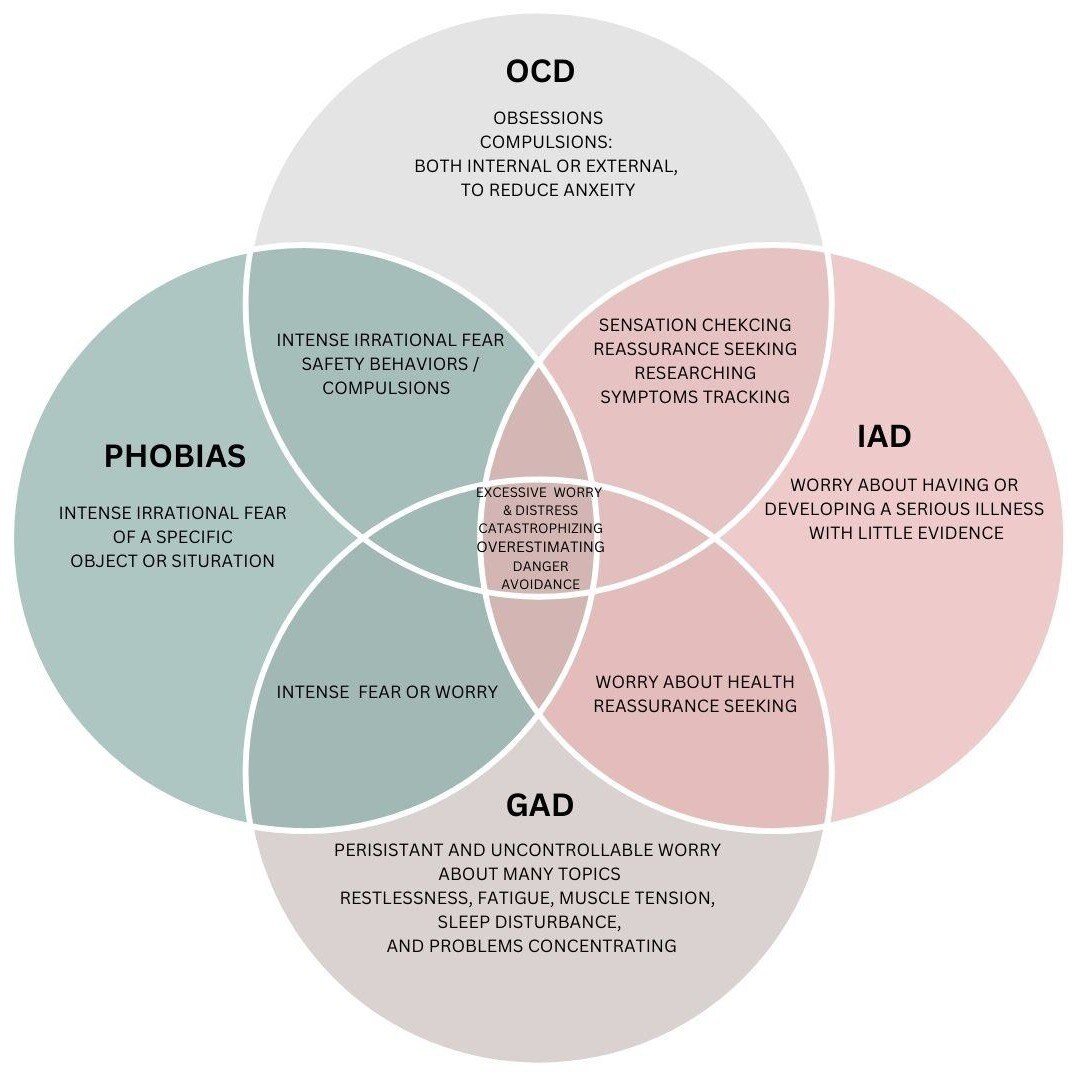
For therapists, grasping the nuanced distinctions between OCD and other anxiety disorders is vital for accurate diagnosis, leading to the most...

In the world of mental health, the roles of Licensed Professional Counselors (LPCs) and Licensed Clinical Social Workers (LCSWs) are not just...

In the hushed confines of therapy rooms, where whispered truths echo and one's inner world unfolds, therapists often find themselves facing an...