It's My Anxiety.
Phew, anxiety, quite a loaded word. Beyond being a topic of much study and interest in the field of mental healthcare, it has become a trending topic...

I chime in with a "Haven't you people ever heard of closing a goddamn door?"
No, it's much better to face these kinds of things with a sense of poise and rationality.
*SIGH*
Panic! A complex interplay of biological, emotional, and psychological factors. Where does this even come from, and why might you be experiencing this?
Like its friend anxiety, panic comes from related brain systems in the amygdala. You feel as though you're in danger, but you're not. The chemicals are chemical-ing, stuff starts to rapid-fire. Oh no, you're feeling anxiety, the swift build up, and then BOOM! Panic attack. Some people even scream from the intensity of the experience.
Though anxiety and panic come from overlapping systems, they are not identical. Think of it this way:
Anxiety is the smoke detector = Anticipatory
Panic is the alarm = Reactionary
Panic being reactionary is why the sensation of it feels so physical, how fun! Let's take a closer look, shall we?
A panic attack happens because your brain is basically an overcaffeinated security guard who takes its job way too seriously. It spots some tiny, harmless internal sensation, maybe your heart skips a beat, maybe you stood up too fast, and, it slams the big red "WE'RE ALL GONNA DIE" button.
This description might be a tad dramatic to non panic sufferers, but it does feel that way, to people who suffer from this disorder.
Suddenly your body is throwing adrenaline around, your heart is sprinting like a lion is chasing, and your lungs are doing its part to keep up. Meanwhile, your thinking brain shows up five seconds late like, "Who started all this?" but by then the alarm is blaring and the whole system is in full meltdown mode. The wild part is that the whole thing was triggered by something as tiny as a bodily hiccup or a sensation so small you might not know what started it, but your brain decided it was time for a full‑scale emergency drill.
One moment you're minding your business, and the next your heart is sprinting, your breathing forgets how to breathe, and your body acts like it's preparing to outrun a bear that absolutely does not exist.
It's the fight‑or‑flight system throwing a surprise party you never asked for, complete with sweaty palms, shaky legs, and a dramatic sense of doom. The whole thing usually peaks fast, fizzles out on its own, and leaves you feeling like you just survived an emotional roller coaster.
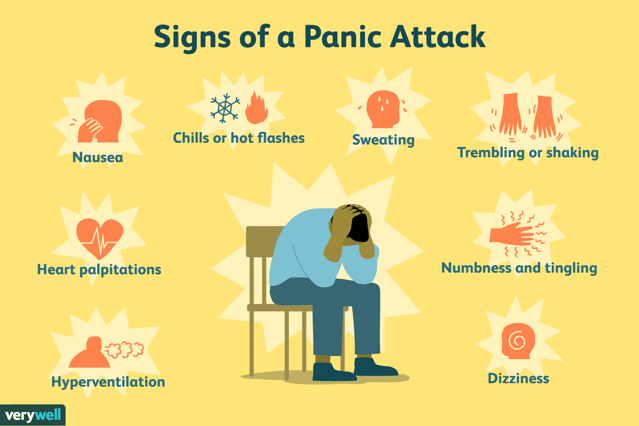
Eventually, the prefrontal cortex shows up like a tired manager who's seen this before and goes, "Okay, everyone calm down, there is nothing happening." Meanwhile, your body is still buzzing with leftover adrenaline like comming down from a car accident, but the parasympathetic nervous system, the body's built‑in chill-out crew, slowly walks in wearing sunglasses and flips the giant switch labeled "Relax, dude."
Your heart rate starts dropping, your breathing remembers how to be normal, and the amygdala sulks in the corner like, "Fine, maybe it wasn't a bear." Within minutes, the whole system powers down, leaving you feeling like you just survived the bear chasing you.
You may laugh, you may cry, but you survived…sitting in your car in the mall parking lot.
You might have a panic disorder.
Those with panic disorder have frequent and unexpected panic attacks. Basically, this happens when your brain’s internal alarm system gets set off.
Your amygdala, remember that guy? The tiny almond-shaped part of your brain in charge of detecting danger, decides that everyday life is actually a high-stakes moments, so it keeps slamming the panic button over everyday random occurrences. Once that button gets hit, your body jumps into fight‑or‑flight like it’s suddenly activating for you to outrun the lion.
Meanwhile, your logical brain shows up late with a clipboard, sees the chaos, and stands there like Michael Scott from The Office.

Really guys? Really?
Over time, your brain starts worrying about the next false alarm, which only makes the alarm system even jumpier. This develops from one random panic attack into a whole system, and suddenly you may find it is an everyday occurrence and eventually, perhaps several times a day. I call it Panic about the panic. (It's like you had a traumatic event with out the actual event.)
AND BEFORE YOU START THE NEGATIVE SELF-TALK: A panic disorder isn’t you “being weak”; it's just your brain being a bit overprotective or having a false alarm.
People often recognize a panic attack by the way it comes on. It’s a mix of strong physical sensations and a sudden rush of fear that doesn’t match what’s happening around them. For some, it builds gradually: maybe your chest feels tight, your breathing shifts, or a wave of uneasiness moves through you, and you can sense something escalating. For others, it arrives quickly, almost like a switch flipped without warning.
The common thread is that your body reacts as if there's immediate danger even though you're actually safe. Your heart may race, your breathing may feel off, your thoughts may speed up, and it can feel overwhelming or confusing. Those sensations can be intense, but they're coming from your body’s alarm system misfiring, not from any actual threat. Over time, many people get better at noticing their early signs, but it's also completely normal if it sometimes feels sudden.

When a panic attack hits, the kindest thing you can do is slow everything down. Take steady, easy breaths and let your feet remind you that you’re standing somewhere safe. It helps to take notice of something real around you: a sound, a texture, the temperature of the air, anything that anchors you back into the present.
If someone you trust is nearby, letting them know you’re overwhelmed can help your nervous system settle. And as the wave rises and falls, which it always does, you can gently remind yourself that your body is reacting to a false alarm, not a real threat. You’re not doing anything wrong, you’re just riding out a moment your brain misinterpreted, and it will pass.
Fortunately/unfortunately panic attacks and panic disorder are more common than many people realize. Panic attacks affect about 2-3% of Americans in a given year. While anyone can experience a panic attack, they occur more frequently in women than in men, and data is unfortunately underrepresented for queer folks. Since panic attacks are tied into anxiety they often begin in early adulthood, but children and adolescents can also be affected.
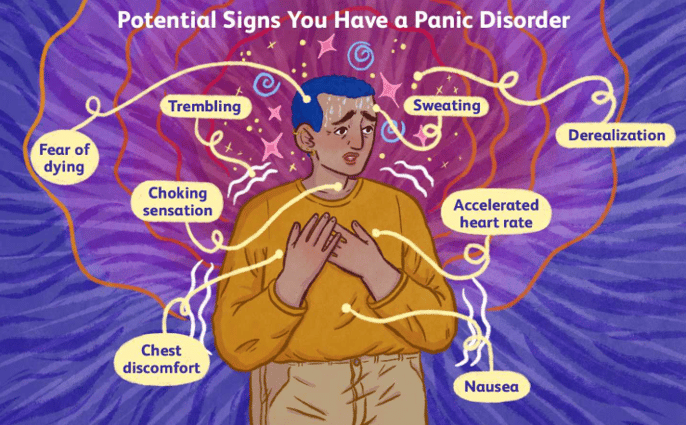
Panic disorder, and subsequently the panic attacks that come with it, can significantly impact a person’s daily life, causing them to avoid certain situations or places out of fear of experiencing another attack. Fortunately, both panic attacks and panic disorder are highly treatable conditions, with therapy and medication proving effective for many people.
Treating panic attacks and panic disorder is kind of like giving your brain a skilled support crew instead of letting it improvise every crisis scene on its own. Getting help for panic disorder can feel intimidating, but reaching out is really just giving yourself a chance to breathe again.
The first step often feels the biggest, not because you’re doing something wrong, but because you’re doing something new. Once you talk to a therapist, doctor, or even a trusted person in your life, the whole process usually feels far less scary than the story your mind built around it. This is a judgement-free zone bestie, you’re giving yourself support, clarity, and tools that make life easier. And the moment you take that step, you’re already proving to yourself that you’re stronger and more capable than the panic ever made you feel.
Therapy steps in like a calm, wise coach who teaches your nervous system that every skipped heartbeat or weird sensation is not a reason to pull the panic lever. Therapists use a few well‑known approaches to help people with panic disorder, each one targeting a different part of the "false alarm" cycle.
One of the most common is Cognitive Behavioral Therapy (CBT), which helps you understand how your thoughts, sensations, and reactions feed into each other, and teaches you new ways to respond when panic shows up. A specific branch of this, exposure‑based therapy, gently helps you face the physical sensations you fear so your brain learns they're uncomfortable, but not dangerous. Some therapists also use interoceptive exposure, which is just a fancy way of saying "practice the sensations in a safe setting so they stop feeling threatening." There's also mindfulness‑based approaches, which help you notice sensations without spiraling into fear, and acceptance‑focused therapies
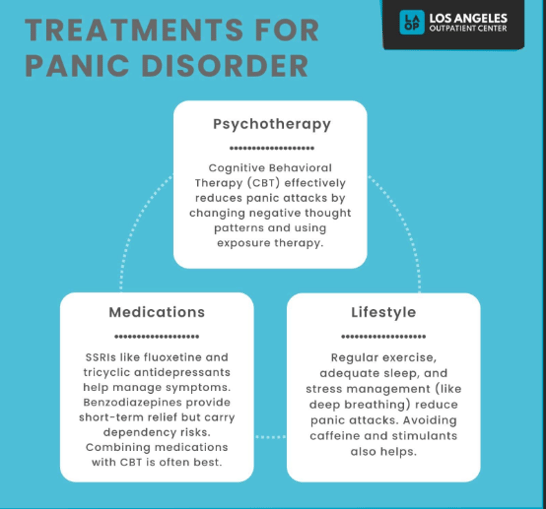
Medication, on the other hand, works more like a quiet backstage technician who adjusts the lighting and sound, so the alarms don’t blast at full volume every time your amygdala gets jumpy.
There are a few main categories of medication that doctors often use to help people with panic disorder, each working on a different part of the body’s alarm system. Antidepressants, especially SSRIs and SNRIs, are commonly used because they help steady the brain’s fear circuits over time, making the alarm system less jumpy.
Another option sometimes used is beta‑blockers, which don’t affect fear directly but can help with the physical symptoms like a racing heart, making the whole experience feel less overwhelming. All of these are tools a healthcare professional might consider based on someone’s needs, and they’re usually most effective when paired with therapy that helps retrain the brain’s response to panic. Together, therapy and medication prescription and management, help your brain stop treating everyday life like a disaster drill and start responding more realistically, so those sudden waves of panic become less frequent, less intense, and a lot less convincing.
Phew, see? Not so bad, huh? Whether you’re ready to address this now, or you’re still trying to figure it out – that is okay. Sometimes this kind of information can feel almost as intense as panic itself. We understand. Knowledge is power!

We are KDH Counseling, located in Lafayette, Louisiana. Here, we offer a warm, professional, and deeply supportive environment for individuals seeking meaningful relief from anxiety and related mental health challenges. Our team of licensed therapists provide a comprehensive range of services including therapy, medication management, and psychological evaluations to children, teens, and adults.
Our practice is staffed by a diverse team of therapists, each with unique specialties, who work collaboratively to tailor treatment to each person’s needs. Clients describe our therapists as empathetic, dedicated, and deeply invested in helping folks move toward healthier, more fulfilling lives.
Our mission is not just to help clients feel better in the moment, but to empower them with the insight, and confidence needed to thrive long‑term in their own way. For folks around Lafayette looking for a place where they can be heard, supported, and guided by skilled professionals who truly care, KDH Counseling offers a path forward, one grounded in expertise, compassion, and a genuine commitment to helping people live more balanced, grounded, and emotionally healthy lives.
Whatever path is right for you, we’re there for you, every step of the way.
Source Material:
Panic Attacks & Panic Disorder: Causes, Symptoms & Treatment
Panic attacks and panic disorder - Symptoms and causes - Mayo Clinic
Panic Disorder: What You Need to Know - National Institute of Mental Health (NIMH)

Phew, anxiety, quite a loaded word. Beyond being a topic of much study and interest in the field of mental healthcare, it has become a trending topic...
What Is EMDR Therapy? A nervous-system healing that starts with how humans process fear. People often arrive in therapy acutely aware of their...

Discover how Brainspotting vs EMDR can be used more efficiently to work with trauma. What is Brainspotting? Branspotting (BSP) therapy is a powerful...